HIP PAIN
- SYOS
- Dec 26, 2021
- 14 min read
Updated: Mar 27, 2022
HIP PAIN
There are many causes of hip pain, affecting different groups of patients from the very young right through to the more aged. Depending on the type of pain you are suffering, different treatment options may be offered. For all types of hip pain a thorough history and examination is essential and further investigations are often required. Sometimes the cause of pain, which appears to be coming from the hip, actually has its origins outside of the hip joint. Correct diagnosis and treatment are therefore essential.
Causes of hip pain:
• Hip arthritis
• Trochanteric bursitis
• Hip fracture
• Snapping tendons
• Cartilage damage
• Troublesome hip replacements
OTHER CAUSES OF HIP PAIN:
• Referred back pain • Avascular necrosi • Developmental problems • Groin pain • Nerve entrapment
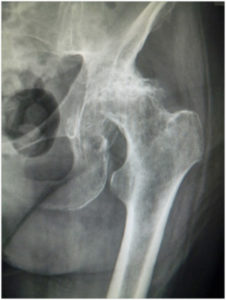
Hip Arthritis Included in this group of patients are those suffering from Osteoarthritis (Fig. 1) or “wear and tear” hip arthritis and inflammatory arthritis, such as rheumatoid arthritis. Whilst patients tend to be older in this group, these conditions may affect almost any age group. The problem is caused by thinning of the joint cartilage leading to pain, restricted movement and a gradually increasing difficulty in performing even the simplest of day-to-day tasks. Pain is commonly experienced deep in the groin and into the thigh. Initially it is usually worse during, or immediately after activity, gradually deteriorating such that pain is experienced with even simple activities such as rising from a chair, going up and down stairs and also in bed at night. If the condition becomes quite severe, patients sometimes notice that they have difficulty standing straight due to stiffness in the hip. It is quite common to have back pain as a result of this. The diagnosis is made by the doctor examining you, but confirmed by an X-ray of the hips. If the diagnosis is unclear, an injection into the hip joint may be undertaken to confirm this as the source of pain.
Initial treatment of an arthritic hip follows simple measures such as painkillers, anti-inflammatory tablets, physiotherapy, activity modification and walking aids (sticks etc.) if necessary. Ultimately, if these methods do not help, a hip arthroplasty (or replacement as it is more commonly known) may be recommended. This is not the first line of treatment as it is a major surgical operation, which carries some risks.

FIG.1Osteoarthritis of the right hip
How bad does the arthritis have to be before you are offered a new hip? Each patient is different – some patients may have few symptoms with advanced hip disease, whilst others suffer more severe problems with less marked disease. The decision is therefore made during a consultation with an appropriately experienced surgeon, where the best decision is made for each person, taking a number of factors into consideration. It is not simply made on how bad an x-ray looks. By this stage simpler forms of treatment are normally failing and you are having increasing pain, which is severely affecting your life.
What exactly is a hip arthroplasty (replacement)? Hip replacements are a very common operation, where an artificial joint replaces your hip joint. They have been successfully undertaken for over fifty years and have a very high patient satisfaction rate. Your hip is replaced in two parts with a ‘cup’ being placed into your worn outer hip socket and a ‘stem’ being placed in your thigh bone with a ‘ball’ placed on top to form a new joint (Fig. 2).

FIG.2An Exeter cemented hip arthroplasty
What is my new hip made of and how is it held in place? The cup is either a single piece of very high grade plastic, which is held in place by specially developed bone cement, or is a metal cup which is impacted in place without cement (uncemented). Either a high grade plastic or ceramic insert is then fitted inside it. The uncemented cups are designed in such a way as to allow your own bone to grow into the back of the cup, so that in time it effectively becomes a part of you. The stem is metal and again is either held with bone cement or is impacted in place to allow the bone to grow into it. Both designs are stable immediately. Either a metal or a ceramic head (ball) is then placed on top of the stem. A combination of both cemented and uncemented fixation may be used in the same patient. Your surgeon will discuss with you and advise you on the type of implant and method of fixation best suited to your requirements. Younger patients with stronger bone are more likely to have an uncemented hip replacement and a ceramic bearing.
What type of hips do you use? All the hip prosthesis used by SYOS surgeons have a proven track record and good reliability. The sockets used are either Ogee, Contemporary or Pinnacle cups, whilst the stem implants are Exeter or Corail. The heads used are either metal or ceramic and are of different sizes, which helps to reduce the risk of your hip replacement dislocating.
How will a hip replacement help me? There are many potential improvements from a replacement hip. The main benefit is a reduction in your pain. Whilst normally there is almost complete relief, you may be left with some mild residual discomfort. Your stiffness is also usually improved significantly and a combination of these benefits may allow you improved function and walking ability. Whilst your movement should improve, it will never return entirely to ‘normal’. If you have noticed your affected leg being shorter then the other side, we are often able to improve this. However, this is not always possible and on occasion a shoe raise is needed after surgery to equalize your leg lengths.
What do I do now? Having decided to undergo a hip replacement, your name will be placed on a waiting list, which allows investigations to be undertaken and also time for you to reflect upon your decision. You will be contacted to organise a pre-assessment visit and also to be informed of the date/time of your surgery. On occasion it may be necessary to organise a review by a Consultant Anaesthetist prior to your operation.
How long will it be before I come in? Unless there is an urgent need to undertake your surgery, you have medical insurance, or are paying for your own medical care, it is likely to be around 6-10 weeks.
FIG.3Avascular necrosis
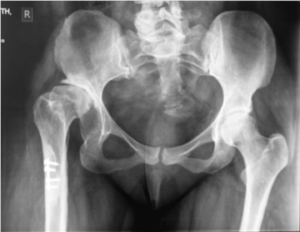
FIG.4Developmental dysplasia – previous dislocation
Is there anything I need to do before my surgery?
Pre-assessment You will be asked to attend for an assessment prior to your admission, where a specially trained nurse will check that you are as fit as you can be for surgery. This allows your health to be checked, swabs taken to ensure you are not carrying certain bugs (MRSA is carried by at least 25% of the population), blood tests are organized and any further tests deemed appropriate (ECG, Chest x-ray etc.)
Medical evaluation A full history and examination are undertaken to ensure any medical conditions you may have are fully evaluated and that treatment is optimized. This may require you to seek further help from your GP or specialist.
Medication review Please bring a list of all your current medications with you to your consultations in the out patient department. Bring all your actual medications with you when you are admitted for surgery. There are some medications, which you may be asked to stop prior to surgery.These include:
• Warfarin • Clopidogerol • HR • oral contraceptive pill
Alternative treatments may be necessary.
Smoking Smoking has a detrimental effect on the body’s healing process and as such, if you do smoke, please try and stop or at least significantly cut down beforehand.
Weight loss If you feel you may need to lose some weight, it would be an ideal time to do so. Weight loss can help your recovery and also reduce the risks of surgery, many of which are significantly increased in patients who are clinically obese. If you have been found to be clinically obese at your outpatient visit and been given a target weight to achieve in order to reduce your surgical risk, your surgery may be postponed if you have not achieved your target.
Exercise Please continue to maintain as much activity as you can prior to surgery, as this will help your recovery afterwards.
Infection Any infections you have anywhere in your body at the time of surgery may potentially spread via your bloodstream to the new hip joint. If you are found to be suffering from an infection, your surgery will be postponed. Examples would include infections of the chest, urinary (water) system, teeth or skin. Your dentist should treat any loose or severely decayed teeth prior to surgery. Skin infections should also be treated by your GP.
Home/social circumstances Whilst you will be able to walk with crutches or a frame, you may need some help with some everyday tasks such as shopping, bathing, cleaning etc. If you live alone, arrangements will be made at your pre-assessment visit to have the necessary help in place for the time of your surgery.
What happens when I come in? You will be taken to your room by a member of staff and then be admitted by one of the nursing team. The anaesthetist will visit you to discuss the best type of anaesthesia for you. This is usually a spinal injection, but may be a general anaesthetic. Your surgeon will also visit you to confirm you still wish to undergo the surgery, discuss the risks and complications again, ask you to sign a consent form and place a mark on the affected leg to ensure the correct side is operated on.
What about consent?
Your surgeon will discuss the potential benefits and risks for your hip replacement surgery. Once you have discussed this fully, you will be asked to sign a consent form.
Potential benefits include: • Improved pain • Improved stiffness • Improved walking ability
Potential risks include: • Infection • Blood clots • Dislocation • Nerve or blood vessel damage • Difference in leg lengths • Swelling of the le • Stiffness of the joint • Fracture of the pelvis or thigh bone • Wear of the artificial joint, loosening and repeat surgery.
What does the surgery involve? Once you have been admitted, checked, consented and marked, you will be taken to the operating department at the appropriate time. You will first be taken to the anaesthetic room to prepare you for your surgery. You will then be positioned lying on your side, to allow the surgery to be undertaken.
How long does it take? The procedure itself takes approximately an hour and a half, but you will be away from you room for about two and a half to three hours.
Can I see my partner/relative after surgery? If you have had a spinal anaesthetic, you should be well enough to see your partner/relative/friend as soon as you return to the ward. It may take a little longer to come round after a general anaesthetic, and if your surgery is in the evening, it is usually better to leave this until the morning.
What about pain? We recognize this is a major surgical procedure and that you are likely to have some pain afterwards. We will do our best to keep this to a minimum. You will be given painkillers at the time of surgery and will be prescribed regular medication to help ease the pain.
When can I get up after surgery As soon as you have recovered from your anaesthetic and have been seen by the physiotherapists, you are able to start mobilising.
What will happen on the first day after the operation? You will be seen by the Physiotherapists, whose job it is to help get you moving safely after your surgery. It is important that you understand their instructions fully, as this will give you a better, quicker recovery and help to minimise the potential complications.
How long will I be in hospital? Not all patients get going at the same rate, but usually you will be in hospital between two to five days.
How will I get home? Part of the physiotherapy assessment prior to discharge is to ensure you are able to get into and out of an appropriate vehicle. Most patients are able to enter a normal car at discharge, although the occasional patient requires a Medicar to take them home.
I live alone – how will I manage? This will be discussed at pre-assessment and the necessary help/ additional support arranged prior to your admission so that it is available for your discharge from hospital.
Do I need to have clips/stitches out afterwards? By far the majority of patients undergoing a hip replacement through SYOS will have a dissolvable suture in place, which does not require removal.
What help will I get to go home? The Physiotherapists and Occupational Therapists will ensure any aids or adaptations which are required will be identified and organized prior to your surgery. This will entail the use of a frame initially and crutches shortly afterwards. Aids to put on socks, stockings or tights, chair and toilet raises to ensure you do not have to bend too much in the early days of your new hip replacement.
What can I do to help my recovery? Within the limitations of range of movement, which will be explained fully to you, you should try and mobilise as much as you feel comfortable to. This will help re-train your muscles, improve your long-term function and reduce the risk of blood clots. Maintaining a healthy balanced diet will also help all these things; in the early days after your surgery, it is advisable to drink plenty of fluids, move your feet/toes as much as possible and not sit down too much to rest – these precautions will help reduce your risk of complications.
What can I/ can’t I do afterwards You should be able to do most things you wish to within reason – we wouldn’t recommend you take up parachuting afterwards! Most activities where the hip is not pushed to the end limits of its range of motion are fine.
How long before I can drive? This depends on your recovery, but most patients are able to drive after six to twelve weeks. You should discuss this with your surgeon at your six-week postoperative review appointment.
Do I need crutches? Yes. These are usually necessary for the first six weeks, but can be reduced as your hip ‘settles down’ and your muscles strengthen. It is important that you follow the guidelines given to you, as should you fall or twist your hip excessively before all the muscles and soft tissues have settled, you may increase your risk of dislocation and the need for further surgery.
Are there any things I should avoid doing? There are some basic precautions you should take for the first three months following your operation:
DO NOT cross your legs DO NOT roll onto or lie on the side OPPOSITE your hip replacement DO NOT bend the operated hip excessivel DO NOT twist or swivel on you operated leg DO NOT bend your operated leg up towards your chin or bend down to reach your feet
When can I fly? What about the airport? We would recommend you do not fly within three months of your surgery, as there is an increased risk of blood clots. Occasionally patients get stopped at metal detectors/ body scanners at the airport due to the metal implant. It is possible to get a card, the Orthocard, through your Surgeon and the Hospital, which confirms you have had joint replacement surgery. This is being increasingly recognized at all UK airports.
What are the risks? As with any surgery there are potential risks involved, including:
Infection
We take this risk very seriously, providing antibiotics during your surgery, operating in special ‘clean air theatres’ only and taking extra precautions throughout your surgery. However, there is still a 1% risk of infection, which can sometimes result in the need to remove your hip replacement and undertake further surgery
Blood clots
– DVT/PE A DVT (Deep Vein Thrombosis) is a blood clot, which may form in the leg following your surgery. If it remains within your leg, this causes swelling and some discomfort, which is usually treated with warfarin therapy. If the clot breaks off and travels to the lungs, this is a Pulmonary Embolus (PE), which can be very serious and is occasionally fatal. Moving your legs on the bed, drinking plenty of fluid to remain hydration and early mobilisation will help to reduce this risk. You will also be given injections into your abdomen whilst in hospital and provided with tablets to take home when you leave, both of which help to ‘thin’ your blood and reduce the risk of clot formation. If suitable, special stockings may need to be worn for six weeks. Not all patients will wear these, as incorrectly fitting stockings can cause increased problems.
Dislocation This is an increased risk within the first three months, until the muscles and soft tissues have healed. This is most likely to happen at the extremes of motion, so please follow the precautions outlined earlier. Repeated dislocations may lead to the need for further surgery, in order to reduce the recurrence. The risk of dislocation is approximately 2%.
Leg length An increase or decrease in the length of your leg may occur. This is often not noticeable by patients, but on occasion may cause problems. At the time of surgery it is sometimes necessary to increase the length to obtain stability. For the majority of people with a leg length difference, a simple shoe insert will balance the lengths and provide a satisfactory solution.
Nerve damage There may be some numbness on the outer aspect of your thigh, related to the surgical scar. This may be temporary or permanent and is unavoidable, but does not cause you any harm. There is a small risk of damage to either the sciatic or femoral nerves, which can leave you with numbness of your foot, the inner aspect of your thigh and/or a foot drop. Usually this is due to a nerve having been stretched and it will recover. However, it may take up to two years to do so. Very occasionally this may be a permanent issue.
Blood transfusion During your surgery, there will be a degree of blood loss. If this is excessive, you may require a transfusion, although every effort is taken to minimise this risk. You may be given a drug called tranexamic acid at the time of surgery, which helps to reduce your blood loss. Jehovah’s witnesses should discuss alternatives to blood transfusion with their surgeon, prior to admission.
Swelling and Stiffness This is usual and may take several weeks or even months to settle.
Catheter Sometimes due to a combination of bed rest, pain relief, surgery and an anaesthetic, patients find it very difficult to pass urine in the first day or two after surgery. If this occurs, a tube called a catheter will be passed into your bladder and will remain there until you are fully mobile and able to pass water normally.
Fracture Very rarely, a small fracture (break in the bone) may occur at the time of surgery. Should this happen, it will be repaired by your surgeon immediately. This may require you following restricted weight bearing activities for a time after surgery, until it has healed
Loosening Over time, the surfaces of your new hip joint may become worn and cause loosening of your new joint. This may cause some pain and the need to undergo revision surgery. It is expected your hip will last you 15 years or more and with newer ceramic type bearing surfaces, this may be considerably longer.
Other causes of hip pain:
Trochanteric bursitis This is due to inflammation and swelling of a small fluid filled sac on the outside of your thigh, over the bony part, which you can feel. This is likely to cause difficulty lying on your side, sleep disturbance and pain on walking, especially on hills/stairs. Usually this does not involve the hip joint itself and treatment includes steroid injections and physiotherapy.
Hip fractures These are acute events, which require emergency treatment. There is almost always a traumatic event such as a fall leading to a fracture of the hip. You will almost certainly be taken directly to Accident and Emergency, where you will be admitted and most likely undergo surgery.
Snapping tendons There are several tendons around the hip joint, which may cause a snapping sensation on certain movements and activities. Such problems are often difficult to diagnose and require careful clinical examination, often followed by specialist imaging. Depending on the source, differing treatment options may be offered.
Troublesome hip replacements If you already have a hip replacement and it is becoming painful, there are many potential causes, including infection, loosening and dislocation. We are able to investigate these causes fully and give advice on the best way to proceed. Not all painful hip replacements require revision surgery, but on occasion this is the only solution.
Referred back pain pain from the lower region of the back may be referred to the hip joint – whilst you may believe the pain you are experiencing is coming directly from your hip joint, it is actually coming from higher up. This may be confusing for some patients, but often helping the back pain improves the groin and hip pain significantly.
Avascular necrosis There are several causes of avascular necrosis (AVN), which may cause significant hip pain, but not be apparent on a simple X-ray. This condition is caused by a reduced blood supply to areas of the hip joint, which may lead to the collapse of the bone. This causes pain. Early cases are diagnosed using an MRI scan and various treatment options are available, although the end result may be a Total Hip Arthroplasty.
Developmental problems If you have had problems with your hip during childhood, either through different development than normal after a dislocated hip as a child, through diseases such as hip infection, Perthes’ disease, Slipped Upper Femoral Capital Epiphysis or due to trauma, it is highly likely you may need further treatment as an adult. Such problems are often complex and require thorough discussion, examination and investigation. Surgery may be challenging, requiring specialist equipment and careful planning.
Vascular problems Occasionally, patients who have significant problems with the flow of blood through their main arteries to the legs, may have pain which is referred into the hip or buttock. This is often a cramp-like pain and comes on after walking short distances. It is usually relieved by rest and often requires referral to a Vascular Surgeon for treatment.
Nerve entrapment Rarely patients have pain around their hip and groin region, together with tingling and/or numbness on the outside of their thigh. This may be caused by pressure on a nerve as it comes underneath the inguinal ligament, at the lower end of the muscles in your abdominal wall. This is termed ‘meralgia paraesthetica” and may require injections or possibly surgical release.







Commentaires